Original Article
Miracle Negative Pressure Wound Therapy (NPWT) or Vacuum Assisted Closure (VAC): For Difficult and Complicated Wounds: An Observational Study
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
New Indian Journal of Surgery 15(3):p 95-100, July-September 2024. | DOI: https://dx.doi.org/10.21088/nijs.0976.4747.15324.1
How Cite This Article:
Sharma A. Miracle negative pressure wound therapy (NPWT) or vacuum assisted closure (VAC): for difficult and complicated wounds: an observational study. New Indian J Surg. 2024;15(3):95-100.Timeline
Abstract
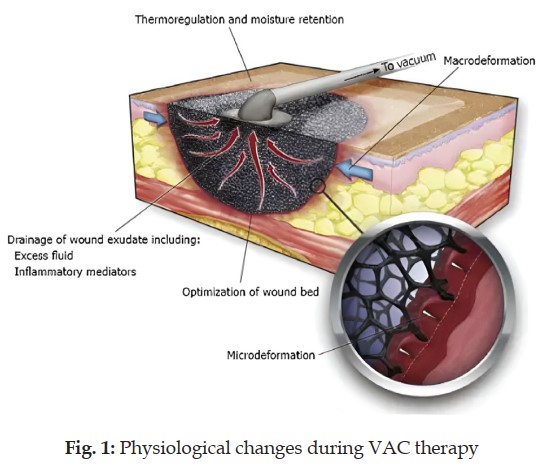
In complicated wounds, healing is a challenge, particularly for the elderly with co-morbidities, which is a major concern. It can lead to prolonged treatment, pain, and morbidity and require major reconstructive procedures, which foist enormous financial and social burdens. Negative pressure wound therapy (NPWT) or vacuum-assisted closure (VAC) is a miracle and more acceptable method as an alternative in wound management that relies on sub atmospheric pressure and encourages the wound for spontaneous healing or by reducing the burden of reconstructive procedures. VAC application methods include thorough debridement, haemostasis, and the application of sterile sponge or foam dressing. A tube with fenestrations is submerged in the sponge, and the wound is wrapped to make it airtight or watertight with adhesive tape. The vacuum pump with fluid collection container is connected to the fenestrate tube. The pump delivers intermittent or continuous suction with pressure ranging from 50-55 to 120-125 mmHg. The NPW dressings are replaced on the third day. Negative pressure therapy reduces wound oedema and bacterial load, stabilizes the wound environment, improves perfusion, and stimulates angiogenesis and granulation tissue. All these mechanisms facilitate the possibility of primary wound closure and reduce the need for other reconstructive procedures. VAC therapy seems to be more effective and simpler than traditional dressings for wound care management in reduction in wound size and volume, depth, treatment duration, and cost.
References
- 1. Morykwas M.J., Argenta L.C., Shelton-Brown E.I., and McGuirt W. Vacuum-assisted closure: a new method for wound control and treatment. Animal studies and a basic foundation. Ann Plast Surg. 1997;38:553–562. [PubMed] [Google Scholar]
- 2. Argenta L.C., Morykwas M.J., Vacuum-assisted closure: a new method for wound control and treatment. Clinical experience. Ann Plast Surg. 1997;38:563-577. [PubMed] [Google Scholar]
- 3. Genecov D.G., Schneider A.M., Morykwas M.J., Parker D., White W.L., and Argenta L.C. A controlled subatmospheric pressure dressing increases the rate of skin graft donor site reepithelialization. Ann Plast Surg. 1998;40:219–225. [PubMed] [Google Scholar]
- 4. Armstrong D.G., Lavery L.A., and Abu-Rumman P. Outcomes of subatmospheric pressure dressing therapy on wounds of the diabetic foot. Ostomy/ Wound Manag. 2002;48:64–68. [PubMed] [Google Scholar]
- 5. Orgill D.P. utilises negative pressure wound therapy on open chest or sternotomy wounds. Ostomy/Wound Manag. 2004;50(11A Suppl):15S 17S. [PubMed] [Google Scholar]
- 6. Orgill D.W., Austen W.G., and Butler C.E. Guidelines for treatment of complex chest wounds with negative pressure wound therapy. Wounds (Suppl.) 2004;16:1–23. [Google Scholar]
- 7. Ellis G.: How to Apply Vacuum-Assisted Closure Therapy Nurs Stand. 2016;30:36–39. [PubMed] [Google Scholar]
- 8. Fleischmann W., Becker U., Bischoff M., and Hoekstra H. Vacuum sealing: indication, technique, and results. Eur J OrthopSurgTraumatol. 1995;5:37–40. [PubMed] [Google Scholar]
- 9. CollingeC., Reddix R. The incidence of wound complications related to negative pressure wound therapy power outages and interruption of treatment in orthopaedic trauma patients. J Orthop Trauma. 2011;25:96–100. [PubMed] [Google Scholar]
- 10. Marks M.W., Argenta L.C., and Thornton J.W. Rapid expansion: experimental and clinical experience. Clin Plast Surg. 1987;14:455–463. [PubMed] [Google Scholar]
- 11. Orgill D.P., Manders E.K., and Sumpio B.E. The mechanisms of action of vacuum-assisted closure: more to learn. Surgery. 2009;146:40–51. [PubMed] [Google Scholar]
- 12. MouësC.M., Vos M.C., van den Bemd G.J., Stijnen T., Hovius S.E. Bacterial load in relation to vacuum-assisted closure wound therapy: a prospective randomised trial. Wound Repair Regen. 2004;12:11–17. [PubMed] [Google Scholar]
- 13. Kairinos N., Voogd A.M., and Botha P.H. Negative-pressure wound therapy II: negative-pressure wound therapy and increased perfusion. Just an illusion? PlastReconstr Surg. 2009;123:601–612. [PubMed] [Google Scholar]
- 14. Hsu S., Thakar R., and Li S. haptotaxis of endothelial cell migration under flow. Methods Mol Med. 2007;139:237–250. [PubMed] [Google Scholar]
- 15. Breen E., Tang K., Olfert M., Knapp A., Wagner P. Skeletal muscle capillarity during hypoxia: VEGF and its activation. High Alt Med Biol. 2008;9:158 166. [PubMed] [Google Scholar]
- 16. Lund T., Wiig H., Reed R.K. Acute post-burn oedema: role of strongly negative interstitial fluid pressure. Am J Physiol. 1988;255:H1069–H1074. [PubMed] [Google Scholar]
- 17. Argenta L.C., Morykwas M.J., Marks M.W., DeFranzo A.J., Molnar J.A., and David L.R. Vacuum-assisted closure: state of clinic art. PlastReconstr Surg. 2006;117:127S–142S. [PubMed] [Google Scholar]
- 18. Venturi M.L., Attinger C.E., Mesbahi A.N., Hess Cl., and Graw K.S. Mechanisms and clinical applications of the vacuum-assisted closure (VAC) device: a review. Am J Clin Dermatol. 2005;6:185 194. [PubMed] [Google Scholar]
- 19. Saxena V., Hwang C.W., Huang S., Eichbaum Q., Ingber D., Orgill D.P. Vacuum-assisted closure: microdeformations of wounds and cell proliferation. PlastReconstr Surg. 2004;114:1086–1098. [PubMed] [Google Scholar]
- 20. Wilkes R.P., McNulty A.K., Feeley T.D., Schmidt M.A., Kieswetter K. Bioreactor for application of subatmospheric pressure to three-dimensional cell culture. Tissue Eng. 2007;13:3003–3010. [PubMed] [Google Scholar]
- 21. Greene A.K., Puder M., and Roy R. Microdeformational wound therapy: effects on angiogenesis and matrix metalloproteinases in chronic wounds of three debilitated patients. Ann Plast Surg. 2006;56:418–422. [PubMed] [Google Scholar]
- 22. Kairinos N., Solomons M., and Hudson D.A., The paradox of negative pressure wound therapy—in vitro studies. J PlastReconstrAesthet Surg. 2010;63:174–179. [PubMed] [Google Scholar]
- 23. Guyton, A.C., eighth ed., Saunders; Philadelphia: 1991. Textbook of Medical Physiology; p. 1014. [Google Scholar]
- 24. Timmers M.S., LeCessie S., Banwell P., and Jukema G.N. The effects of varying degrees of pressure delivered by negative-pressure wound therapy on skin perfusion. Ann Plast Surg. 2005;55:665–671. [PubMed] [Google Scholar]
- 25. Fang R., Dorlac W.C., and Flaherty S.F. Feasibility of negative pressure wound therapy during intercontinental aeromedical evacuation of combat casualties. J Trauma. 2010;69(suppl 1):S140–S145. [PubMed] [Google Scholar]
- 26. Borgquist O., Ingemansson R., and Malmsjö M. The influence of low and high pressure levels during negative-pressure wound therapy on wound contraction and fluid evacuation. PlastReconstr Surg. 2011;127:551–559. [PubMed] [Google Scholar]
- 27. Morykwas M.J., Argenta L.C., Shelton-Brown E.I., and McGuirt W. Vacuum-assisted closure: a new method for wound control and treatment. Animal studies and a basic foundation. Ann Plast Surg. 1997;38:553–562. [PubMed] [Google Scholar]
- 28. Morykwas M.J., Faler B.J., Pearce D.J., and Argenta L.C. Effects of varying levels of subatmospheric pressure on the rate of granulation tissue formation in experimental wounds in swine. Ann Plast Surg. 2001;47:547–551. [PubMed] [Google Scholar]
- 29. Kairinos N., Solomons M., and Hudson D.A., Negative-pressure Wound Therapy I: The Paradox of Negative-Pressure Wound Therapy. PlastReconstr Surg. 2009;123:589–598. discussion 599–600. [PubMed] [Google Scholar]
- 30. Streubel P.N., Stinner D.J., and Obremskey W.T. Use of negative-pressure wound therapy in orthopaedic trauma. J Am AcadOrthop Surg. 2012;20:564-574. [PubMed] [Google Scholar]
- 31. ApelqvistJ., Armstrong D.G., Lavery L.A., Boulton A.J., Resource utilisation and economic costs of care based on a randomised trial of vacuum assisted closure therapy in the treatment of diabetic foot wounds. Am J Surg. 2008;195:782–788. [PubMed] [Google Scholar]
- 32. Philbeck T.E., Jr., Whittington K.T., Millsap M.H., Briones R.B., Wight D.G., Schroeder W.J. The clinical and cost-effectiveness of externally applied negative pressure wound therapy in the treatment of wounds in home healthcare medical patients. Ostomy/Wound Manag. 1999;45:41–50. [PubMed] [Google Scholar]
Data Sharing Statement
Funding
Author Contributions
Ethics Declaration
Acknowledgements
Conflicts of Interest
About this article
Cite this article
Sharma A. Miracle negative pressure wound therapy (NPWT) or vacuum assisted closure (VAC): for difficult and complicated wounds: an observational study. New Indian J Surg. 2024;15(3):95-100.
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
| Received | Accepted | Published |
|---|---|---|
| August 07, 2024 | September 12, 2024 | September 30, 2024 |
DOI: https://dx.doi.org/10.21088/nijs.0976.4747.15324.1
Keywords
VAC (vacuum-assisted closure)Negative pressure wound therapy (NPWT)Complicated and difficult woundsLow costSub-atmospheric pressure dressingSearch for Similar Articles
Similar Articles
- Laparoscopic Repair of Large Recurrent Bochdalek Hernia: Case Report with Review...
- A Retrospective Evaluation of Superior Efficacy in Irrigation and Flushing of Sa...
- Implementation of Enhanced Recovery After Surgery (ERAS) Protocols in Elective C...
- Accuracy of TIRADS Classification in the Risk Stratification of Thyroid Swelling...
- Case Series Analysis of Medical Expulsive Therapy in Ureteric Calculi
Article Level Metrics
Last UpdatedSaturday 28 February 2026, 21:28:32 (IST)
Accesses
Citations
Download citation
Article Keywords
Keyword Highlighting
Highlight selected keywords in the article text.
Timeline
| Received | August 07, 2024 |
| Accepted | September 12, 2024 |
| Published | September 30, 2024 |
licence
This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.