Original Article
Effect of Perioral Stimulation, Vertebral Pressure, Abdominal Co-Contraction and Manual Pressure Techniques Along with Chest Physiotherapy on Ventilatory Parameters
Niraj Kumar, Sharon Ashley Sherring, Surbhi Thapliyal, Manju Nautiyal, Ravindra Singh
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
Physiotherapy and Occupational Therapy Journal 17(4):p 213-222, October-December 2024. | DOI: http://dx.doi.org/10.21088/potj.0974.5777.17424.4
How Cite This Article:
Sherring SA, Thapliyal S, Kumar N, Juyal D. Effect of perioral stimulation, vertebral pressure, abdominal co-contraction and manual pressure techniques along with chest physiotherapy on ventilatory parameters. Physio and Occ Therapy Jr. 2024;17(4):213-222.Timeline
Abstract
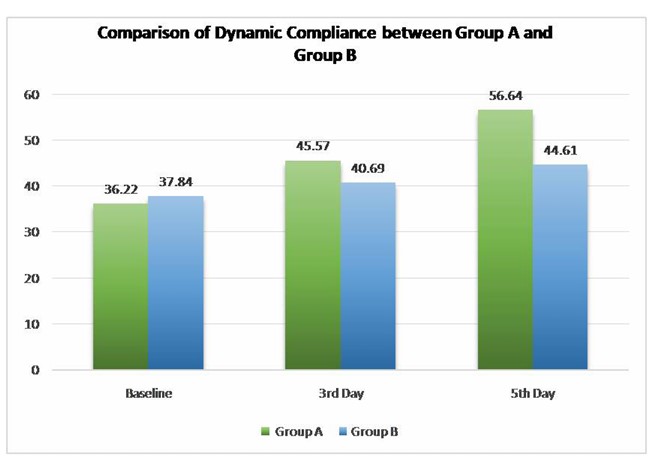
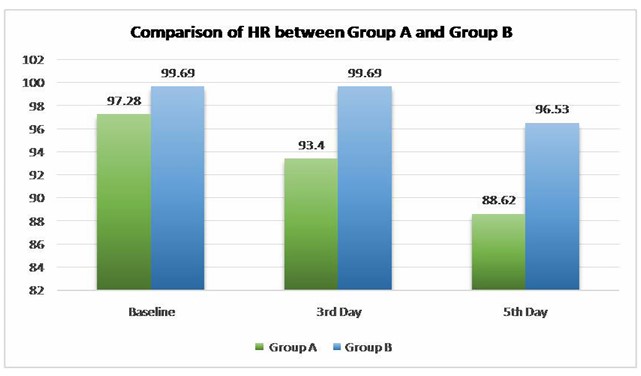
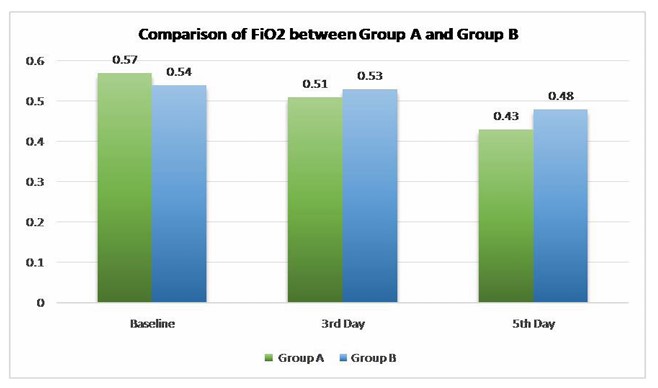
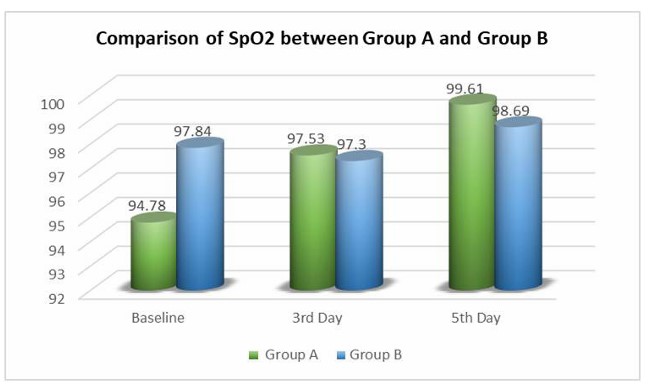
Introduction: Ventilation is the essential part of life. The Intensive Care Unit (ICU) is a specialized department designed for patients with severe or life-threatening conditions, injuries or complications, offering focused management and care for these critical situation Patients on mechanical ventilation usually have larger amounts of pulmonary secretions due to impairment in mucociliary function and compromised mucus transport. Chest Proprioceptive Neuromuscular Facilitation (PNF) is one of the physiotherapy intervention in which proprioceptive and tactilestimuli are given externally to the patient, which produces reflex movement responses of respiration andregulate breathing. Aim: To examine the effectiveness of Perioral Stimulation, Vertebral Pressure, Abdominal Co-Contraction, and Manual Pressure when combined with Chest Physiotherapy compared to Chest Physiotherapy alone and their efficacy in optimizing the weaning process for patients on SIMV mode Procedure: A Randomized control Trial, single-blinded study was carried on 26 participants from Intensive Care Unit. They were then divided into two groups. In Group A participants were treated by PNF and chest physiotherapy and in Group B with chest physiotherapy alone. The interventions were given twice a day for 5 days. The effects on ventilatory parameters (Dynamic Compliance, HR, SpO2, RR, FiO2) were measured and compared from baseline day 1 to day 5. Result: Post-intervention, there was Improvement in Dynamic Lung Compliance, Saturation of Oxygen, Heart Rate, Respiratory Rate, Fraction of Inspired Oxygen in both groups but on Comparing overall improvement, Group A was more effective than Group B. Conclusion: The present study concludes that Perioral Stimulation, Vertebral Pressure, Abdominal Co-Contraction, and Manual Pressure with chest Physiotherapy are better and effective in improving Dynamic pulmonary compliance, saturation of oxygen, and reduction of Heart Rate, Respiratory Rate and FiO2 and lead to early weaning of patients.
References
- 1. Chatburn, Robert L., and M. D. Lough. “Mechanical ventilation.” Pediatric Respiratory Therapy, 3rd ed.; Mandu Press LTD: Cleveland, OH, USA (2003).
- 2. Chang, D. W. (2013). Clinical application of mechanical ventilation. Cengage Learning.
- 3. Leigh JM, Tytler JA. Admissions to the intensive care unit after complications of anaesthetic techniques over 10 years. Anaesthesia ;1990 82–45:8140.
- 4. Pryor, Jennifer A., and Ammani S. Prasad. Physiotherapy for respiratory and cardiac problems: adults and paediatrics. Elsevier Health Sciences, 2008.
- 5. Nagata, I., Takei, T., Hatakeyama, J., Toh, M., Yamada, H., & Fujisawa, M. (2019). Clinical features and outcomes of prolonged mechanical ventilation: a single-center retrospective observational study. JA Clinical Reports, 5(1), 1-8.
- 6. Esteban A, Anzueto A, Alia I, et al. How is mechanical ventilation employed in the intensive care unit. An international utilization reviews. American Journal of Respiratory and Critical Care Medicine. 2000; vol.161, (5): pp1450-1458.
- 7. Radermacher, P., Santak, B., Wüst, H. J., Tarnow, J., & Falke, K. J. (1990). Prostacyclin for the Treatment of Pulmonary Hypertension in the Adult Respiratory Distress Syndrome. Anesthesiology, 72(2), 238–244. doi:10.1097/00000542-199002000-00005
- 8. Burtin C, Clerckx B, Robbeets C, et al. Early exercise in criti cally ill patients enhances short-term functional recovery. Crit Care Med 2009;37(9):2499e505.
- 9. Allen C, Glasziou P, Del MC. Bed rest: a potentially harmful treatment needing more careful evaluation. Lancet 1999;354(9186):1229 1233. PubMed: 10520630
- 10. Yende S, Waterer GW, Tolley EA, et al. Inflammatory markers are associated with ventilatory limitation and muscle dysfunction in obstructive lung disease in well functioning elderly subjects. Thorax 2006;61(1):10–16. PubMed: 16284220
- 11. Duscha BD, Annex BH, Green HJ, Pippen AM, Kraus WE. Deconditioning fails to explain peripheral skeletal muscle alterations in men with chronic heart failure. J Am Coll Cardiol 2002;39(7):1170–1174. PubMed: 11923042
- 12. Bersten A, Soni N. Oh’s Intensive Care Manual. 6th ed. Philadelphia: Butterworth Heinemann; 2009
- 13. Burtin C, Clerckx B, Robbeets C, et al. Early exercise in criti cally ill patients enhances short-term functional recovery. Crit Care Med 2009;37(9):2499e505.
- 14. Ciesla ND. Chest physical therapy for patients in the intensive care unit. Phys Ther. 1996;76(6):609-625. doi:10.1093/ptj/76.6.609
- 15. Barbara A. Webber, Jennifer A. Pryor. Neurophysiological Facilitation of respiration. Physiotherapy for respiration and cardiac problems; 1993, 2nd Edition; Page no. 163-166.
- 16. Chordiya SS, Dr. Atharuddin Kazi, Dr. Akshaya Shetty, Dr. Sambhaji Gunjal, Dr. Maria Lamuvel, Dr. Tejashee Bhoir Effect of respiratory proprioceptive neuromuscular facilitation technique with chest physiotherapy in mechanically ventilated Organophosphorus poisoning patients. International Journal of Multidisciplinary Research and Development Volume 4; Issue 6; June 2017; Page No. 01-06.
- 17. Prajapati H. Effect of Neurophysiological Facilitation NPF of Respiration on Ventilation of Mechanically Ventilated Patients: An Experimental Study, International Journal of Science and Research (IJSR), Volume 7 Issue 9, September 2018.
- 18. Paulraj M, Shristhudhi S, Supriya K, Vinod, Anandbabu K. Effectiveness of PNF of respiration to improve the exercise capacity in patients with COPD: A pilot study. Int J World Res. 2017;1(35):1–6
- 19. Palekar, Tushar J. “Effect of Chest Proprioceptive Neuromuscular Facilitation versus Body Positioning in Mechanically ventilated patients: A cross over study.” Cosmos Impact Factor-5.86 ISSN 2249-3352 (P) 2278-0505 (E), www. pragatipublication.com.
- 20. Castro AA, Calil SR, Freitas SA, Oliveira AB, Porto EF. Chest physiotherapy effectiveness to reduce hospitalization and mechanical ventilation length of stay, pulmonary infection rate and mortality in ICU patients. Respir Med. 2013 Jan;107(1):68-74. doi: 10.1016/j. rmed.2012.09.016. Epub 2012 Oct 22. PMID: 23085215.
- 21. Chang A, Paratz J, Rollston J. Ventilatory effects of neurophysiological facilitation and passive movement in patients with neurological injury.Australian journal of physiotherapy. 2002 Jan 1;48(4):305-10
- 22. Guérin C, Reignier J, Richard JC, Beuret P, Gacouin A, Boulain T, Mercier E, Badet M, Mercat A, Baudin O, Clavel M, Chatellier D, Jaber S, Rosselli S, Mancebo J, Sirodot M, Hilbert G, Bengler C, Richecoeur J, Gainnier M, Bayle F, Bourdin G, Leray V, Girard R, Baboi L, Ayzac L., PROSEVA Study Group. Prone positioning in severe acute respiratory distress syndrome. N Engl J Med. 2013 Jun 06;368(23):2159-68
- 23. Martinez, B. P., Marques, T. I., Santos, D. R., Salgado, V. S., Nepomuceno Júnior, B. R., Alves, G. A., Gomes Neto, M., & Forgiarini Junior, L. A. (2015). Influence of different degrees of head elevation on respiratory mechanics in mechanically ventilated patients. Revista Brasileira de terapia intensiva, 27(4), 347–352. https://doi.org/10.5935/0103-507X.20150059.
- 24. Goerl, K., & Goerl, J. (2016). “The effects of spinal manipulation on heart rate and blood pressure.”Journal of Manipulative and Physiological Therapeutics, 39(8), 589-596. doi:10.1016/j.jmpt.2016.06.005
- 25. Kroeling, P., et al. (2011). “Effects of manual therapy on autonomic function and cardiovascular parameters.” Manual Therapy, 16(3), 220-228. doi: 10.1016/j.math.2010.11.002
- 26. Abhinav Salve, Sachin Maghade, Sneha Katke, Ronald Prabhakar, Mahendra. Effect of Vertebral Pressure Technique and Intercostal Stretch Technique on Respiratory Rate, Tidal Volume, SpO2 and HR.
- 27. Nitz J, Burke B. A study of the facilitation of respiration in myotonic dystrophy. Physiotherapy Res Int. 2002; 7(4):228-38. doi: 10.1002/pri.262. PMID: 12528578.
- 28. Thakkar NB. Role of PNF techniques in chest physiotherapy. Physiotherapy - The Journal of Indian Association of Physiotherapists. 2006 Apr;10-14.
- 29. Gupta p, Nambi G.S, Gupta G. Effects of intercostal stretch technique and anterior basal lift technique on respiratory rate, saturation of peripheral oxygen and heart rate among ICU patients. International Journal of death and science and research, vol.4; issue 2; feb 2014.
- 30. Magee DJ. Orthopedic physical assessment-E Book. Elsevier Health Sciences; 2014 Mar 25. 8(525).
- 31. Bethune DD. Neurophysiological facilitation of breathing in the unconscious adult patient. Physiotherapy Canada. 1975;5:241-5.
Data Sharing Statement
Funding
Author Contributions
Ethics Declaration
Acknowledgements
Conflicts of Interest
About this article
Cite this article
Sherring SA, Thapliyal S, Kumar N, Juyal D. Effect of perioral stimulation, vertebral pressure, abdominal co-contraction and manual pressure techniques along with chest physiotherapy on ventilatory parameters. Physio and Occ Therapy Jr. 2024;17(4):213-222.
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
| Received | Accepted | Published |
|---|---|---|
| November 04, 2024 | December 11, 2024 | December 24, 2024 |
DOI: http://dx.doi.org/10.21088/potj.0974.5777.17424.4
Keywords
Chest PNFerioral stimulationThoracic pressureabdominal Co-contractionManual pressureICUMechanical VentilationSIMVSearch for Similar Articles
Similar Articles
- Exploring the Connection Between Stress, Anxiety, and Central Pain Mechanisms
- Comparative Effectiveness of Mulligan SNAGs and the McKenzie Method in the Mana...
- To Compare the Effectiveness of Dual Task Training Versus Task Oriented Circuit...
- Role of Virtual Reality in Physiotherapy
- Normative Values of One Leg Stance in Urban Adults of 20-40 Years
Article Level Metrics
Last UpdatedSaturday 28 February 2026, 04:25:31 (IST)
Accesses
Citations
Download citation
Article Keywords
Keyword Highlighting
Highlight selected keywords in the article text.
Timeline
| Received | November 04, 2024 |
| Accepted | December 11, 2024 |
| Published | December 24, 2024 |
licence
This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.