Case Report
Assessment of the Analgesic Efficacy of Alkalinized Heparin and Lignocaine in Pain Attenuation During Burn Dressing Changes
Ravi Kumar Chittoria, Divya Darshan, Amrutha J.S., Sriram V.S
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
Journal of Plastic Surgery and Transplantation 5(2):p 63-68, July - Dec. 2025. | DOI: n.a
How Cite This Article:
Divya Darshan, Ravi Kumar Chittoria, Amrutha J.S. et al, Assessment of the Analgesic Efficacy of Alkalinized Heparin and Lignocaine in Pain Attenuation During Burn Dressing Changes. J of Pla Sur and Trans. 2025; 5(2): 63-68.Timeline
Abstract
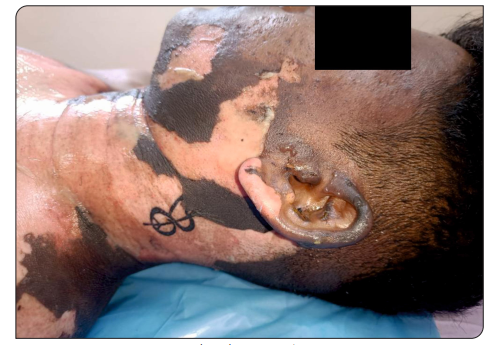
Heparin possesses anti-inflammatory, antihistaminic, anti-allergic, serotoninblocking, and proteolytic enzyme-inhibiting properties. Topical forms of heparin have been used in burn care to prevent burn wound extension, minimize skin tissue loss, promote faster healing with fewer contractures, relieve pain, reduce tissue edema and exudation, prevent infection, and support revascularization, granulation, and epithelialization of deeply burned tissue. Similarly, topical lignocaine in gel form has been applied to raw burn areas and post-skin graft sites, showing significant effectiveness in pain relief. In addition to analgesia, lignocaine has also been shown to reduce edema and post-burn ischemia. In this case report, we discuss the combined use of topical heparin and local anesthetic as part of burn wound management.
References
- 1. Teot L, Otman S, Brancati A, Mittermayr R. Burn scar treatment. In: Kamolz LP, Jescheke MG, Horch RE, Küntscher M, Brychta P, editors. Handbook of Burns. Vienna: Springer; 2012. p. 5567.
- 2. Masoud M, Wani AH, Darzi MA. Topical heparin versus conventional treatment in acute burns: a comparative study. Indian J Burns 2014;22: 4350.
- 3. Catherine J. Sinnott, B.A.Joseph M. Garfield, M.D.Johannes G. Thalhammer, D.V.M.; Gary R. Strichartz, Ph.D. Addition of Sodium Bicarbonate to Lidocaine Decreases the Duration of Peripheral Nerve Block in the Rat. Anesthesiology October 2000, Vol. 93, 1045– 1052.
- 4. C. Lowell Parsons; Paul Zupkas; Jeffrey Proctor; James Koziol; Amie Franklin; Dennis Giesing; Edward Davis; Charles M. Lakin; Bruce S. Kahn; William J. Garner (2012). Alkalinized Lidocaine and Heparin Provide Immediate Relief of Pain and Urgency in Patients with Interstitial Cystitis., 9(1), 207–212.
- 5. Alrich EM. The effect of heparin on the circulating blood plasma and proteins in experimental burns. Surgery 1949;25: 67680.
- 6. Lu J, Xu T, Yang M, Xu XW, Wu B. Heparin for the treatment of burns (Protocol). Cochrane Database Syst Rev 2011;12:CD009483.
- 7. Reyes A, Astiazaran JA, Chavez CC, Jaramillo F, Saliba MJ. Burns treated with and without heparin: controlled use in a thermal disaster. Ann Burns Fire Disasters 2001;14: 183-91.
- 8. Saliba MJ Jr, editor. The Effects of Heparin in the Treatment of Burns. Proceedings of International Meeting; 1994 Feb 24-27.
- 9. Vijayakumar C, Prabhu R, Senthil Velan M, et al. (August 17, 2018) Role of Heparin Irrigation in the Management of Superficial Burns with Special Reference to Pain Relief and Wound Healing: A Pilot Study. Cureus 10(8): e3157.
- 10. Saliba MJ Jr, Dempsey WC, Kruggel JL. Large burns in humans. Treatment with heparin. JAMA 1973;225: 261-9.
- 11. Ferreira Chacon JM, Mello de Andrea ML, Blanes L, Ferreira LM. Effects of topical application of 10,000 IU heparin on patients with perineal dermatitis and seconddegree burns treated in a public pediatric hospital. J Tissue Viability 2010;19: 150-8.
- 12. Elsayed E, Becker RC. The impact of heparin compounds on cellular inflammatory responses: a construct for future investigation and pharmaceutical development. J Thromb Thrombolysis 2003;15: 11-8.
- 13. Saliba M.J. Heparin in the treatment of burns: A review. Burns. 2001;27: 348-357.
- 14. Rayes A., Astiazaran J.A., Chavez C.C., Jaramilla F., Saliba M, J. Burns treated with and without heparin: Controlled use in a thermal disaster. Annals of Burns and Fire Diasters. 2001;14: 183-191.
- 15. Vigneault L, turgeon AF, Côté D, Lauzier F, Zarychanski R, Moore L, et al. Perioperative intravenous lidocaine infusion for postoperative pain control: a meta-analysis of randomized controlled trials. Can J Anesth Can Anesth. 2011 Jan 1;58(1):22-37.
- 16. Wasiak J, Spinks A, Costello V, Ferraro F, Paul E, Konstantatos A, et al. Adjuvant use of intravenous lidocaine for procedural burn pain reliet: A randomized double-blind, placebocontrolled, cross-over trial. Burns. 2011 Sep;37(6):951-7.
- 17. Wasiak J, Mahar PD, McGuinness SK, Spinks A, Danilla S, Cleland H, et al. Intravenous lidocaine for the treatment of background or procedural burn pain. Cochrane Database of Systematic Reviews.Chisester, UK: John Wiley & Sons, Ltd; 2014
- 18. B T Brofeldt 1, P Cornwell, D Doherty, K Batra, R A Gunther, Topical lidocaine in the treatment of partial-thickness burns, J Burn Care Rehabil.,1989 Jan-Feb;10(1):63-8.
Data Sharing Statement
Funding
Author Contributions
Ethics Declaration
Acknowledgements
Conflicts of Interest
About this article
Cite this article
Divya Darshan, Ravi Kumar Chittoria, Amrutha J.S. et al, Assessment of the Analgesic Efficacy of Alkalinized Heparin and Lignocaine in Pain Attenuation During Burn Dressing Changes. J of Pla Sur and Trans. 2025; 5(2): 63-68.
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
| Received | Accepted | Published |
|---|---|---|
| May 06, 2025 | July 21, 2025 | December 30, 2025 |
DOI: n.a
Keywords
Topical HeparinLignocaineAlkalinizedBurnWoundManagement.Search for Similar Articles
Similar Articles
- Surgical Wound Nursing Care: An Integrative Review of Evidence Based Practice
- Diabetic Ulcer Nursing Care: An Integrated Evidence Based Approach
- Role of Cyclical Negative Pressure Wound Therapy in Burn Patients
- Management of Ischial Pressure Ulcer Using Hatchet Flap: Case Report
- Octenidine in Wound Antisepsis: A Review
Article Level Metrics
Last UpdatedSaturday 28 February 2026, 09:57:35 (IST)
Accesses
Citations
Download citation
Article Keywords
Keyword Highlighting
Highlight selected keywords in the article text.
Timeline
| Received | May 06, 2025 |
| Accepted | July 21, 2025 |
| Published | December 30, 2025 |
licence
This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.