Original Article
From Artificial Limbs to Intelligent Limbs: Advances in Sensory-Enabled Prosthetic Technology
L. Lishma Shann Mathew, Vasantha Kalyani
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
International Journal of Practical Nursing 13(3):p 87-99, Sept. Dec. 2025. | DOI: 10.21088 ijpn.2347.7083.13325.
How Cite This Article:
L. Lishma Shann Mathew, C. Vasantha Kalyani. From Artificial Limbs to Intelligent Limbs: Advances in SensoryEnabled Prosthetic Technology. Int J Practical Nurs. 2025; 13(3): 87-99.Timeline
Abstract
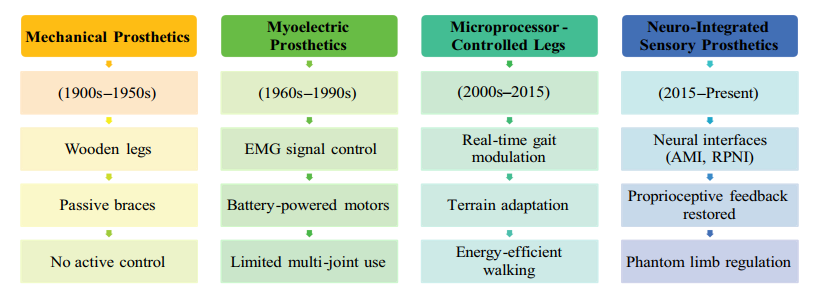
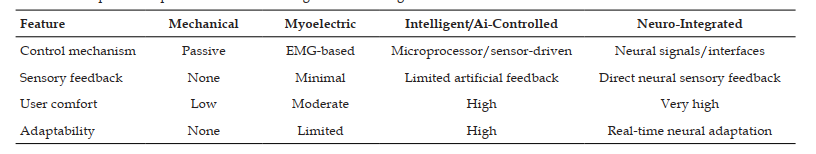
Prosthetic technology has progressed dramatically over the last century, transforming from rudimentary mechanical limbs to modern devices that restore sensory and motor capabilities. Initial prosthetic limbs mostly provide structural support without replicating biological function. Advancements in neural interfaces and surgical techniques, notably the agonist antagonist myoneural interface (AMI), have enabled prosthetics to leverage neuromuscular feedback, hence improving walking speed and gait adaptation. Moreover, progress in machine learning and materials science has resulted in intelligent prosthetics that can respond to human goals, providing real-time modifications to mechanical outputs. The historical evolution of prostheses can be delineated into four phases: mechanical supports, myoelectric control utilizing muscle signals, intelligent prosthetics incorporating sensors and adaptive algorithms, and biohybrid systems that amalgamate biological components with robotics. Post-amputation sensory loss impairs critical feedback systems, requiring the incorporation of artificial sensory pathways in contemporary prosthetics to improve stability and diminish dependence on visual signals. Rehabilitation has progressed to include immersive virtual and augmented reality technologies, which aid functional recovery and increase user engagement with prosthetic devices. Despite the clear advantages of improved prostheses, obstacles persist regarding accessibility, affordability, and the requirement for skilled practitioners. Future advances are anticipated to focus on the integration of more intricate sensory modalities and the creation of resilient, self-repairing materials. Interdisciplinary collaboration will be crucial in surmounting existing obstacles and enhancing the quality of life for prosthetic users, ensuring that devices are both functionally efficient and conducive to identity and autonomy.
References
- 1. Song H, Hsieh TH, Yeon SH, et al. Continuous neural control of a bionic limb restores biomimetic gait after amputation. Nat Med. 2024;30(7):2010-2019. doi:10.1038/s41591-024- 02994-9.
- 2. Massachusetts Institute of Technology. A prosthesis driven by the nervous system helps people with amputation walk naturally. MIT McGovern Institute; 2024.
- 3. Hernigou P. Ambroise Paré IV: The early history of artificial limbs (from robotic to prostheses). Int Orthop. 2013;37(6):1195-1197. doi:10.1007/s00264-013-1884-7.
- 4. Radford M. The history and development of prosthetics. J Prosthet Orthot. 2019; 31(2):102–109.
- 5. Bhuyan, D., & Kumar, K. (2019). A Brief History of Prosthetics and Orthotics of the Lower Body and Their Types (pp. 365–380). IGI Global. https://doi.org/10.4018/978-1-5225-8235-9. CH002.
- 6. Geethanjali P. Myoelectric control of prosthetic hands: state-of-the-art review. Med Devices (Auckl). 2016;9:247-255. Published 2016 Jul 27. doi:10.2147/MDER.S91102.
- 7. Zuo KJ, Olson JL. The evolution of functional hand replacement: From iron prostheses to hand transplantation. Plast Surg (Oakv). 2014;22(1):44-51.
- 8. Roche, A.D., Rehbaum, H., Farina, D. et al. Prosthetic Myoelectric Control Strategies: A Clinical Perspective. Curr Surg Rep 2, 44 (2014). https://doi.org/10.1007/s40137-013- 0044-8.
- 9. Antfolk C, D’Alonzo M, Rosén B, Lundborg G, Sebelius F, Cipriani C. Sensory feedback in upper limb prosthetics. Expert Rev Med Devices. 2013;10(1):45-54. doi:10.1586/ erd.12.68.
- 10. Jayaraman C, Mummidisetty CK, Albert MV, et al. Using a microprocessor knee (C-Leg) with appropriate foot transitioned individuals with dysvascular transfemoral amputations to higher performance levels: a longitudinal randomized clinical trial. J Neuroeng Rehabil. 2021;18(1):88. Published 2021 May 25. doi:10.1186/s12984-021-00879-3.
- 11. Kannenberg A, Zacharias B, Pröbsting E. Benefits of microprocessor-controlled prosthetic knees to limited community ambulators: systematic review. J Rehabil Res Dev. 2014;51(10):1469-1496. doi:10.1682/ JRRD.2014.05.0118.
- 12. Yildiz KA, Shin AY, Kaufman KR. Interfaces with the peripheral nervous system for the control of a neuroprosthetic limb: a review. J Neuroeng Rehabil. 2020;17(1):43. Published 2020 Mar 10. doi:10.1186/s12984-020-00667-5.
- 13. Osborn LE, Moran CW, Johannes MS, et al. Extended home use of an advanced osseointegrated prosthetic arm improves function, performance, and control efficiency. J Neural Eng. 2021;18(2):10.1088/1741- 2552/abe20d. Published 2021 Mar 8. doi:10.1088/1741-2552/abe20d.
- 14. Sensinger JW, Dosen S. A Review of Sensory Feedback in Upper-Limb Prostheses From the Perspective of Human Motor Control. Front Neurosci. 2020;14:345. Published 2020 Jun 23. doi:10.3389/fnins.2020.00345.
- 15. Sando IC, Leach MK, Woo SL, et al. Regenerative Peripheral Nerve Interface for Prostheses Control: Electrode Comparison. J Reconstr Microsurg. 2016;32(3):194-199. doi:10.1055/s-0035-1565248.
- 16. Sun L, Yu Y, Chen Z, et al. Biohybrid robotics with living cell actuation. Chem Soc Rev. 2020;49(12):4043-4069. doi:10.1039/ d0cs00120a.
- 17. Hsiao SS, Fettiplace M, Darbandi B. Sensory feedback for upper limb prostheses. Prog Brain Res. 2011;192:69-81. doi:10.1016/B978-0-444- 53355-5.00005-1.
- 18. Ganesh Kumar N, Kung TA, Cederna PS. Regenerative Peripheral Nerve Interfaces for Advanced Control of Upper Extremity Prosthetic Devices. Hand Clin. 2021;37(3):425- 433. doi:10.1016/j.hcl.2021.04.005.
- 19. Raspopovic S, Capogrosso M, Petrini FM, et al. Restoring natural sensory feedback in real-time bidirectional hand prostheses. Sci Transl Med. 2014;6(222):222ra19. doi:10.1126/ scitranslmed.3006820. 20. Zbinden J, Molin J, Ortiz-Catalan M. Deep Learning for Enhanced Prosthetic Control: Real-Time Motor Intent Decoding for Simultaneous Control of Artificial Limbs. IEEE Trans Neural Syst Rehabil Eng. 2024; 32: 1177-1186. doi:10.1109/TNSRE.2024.3371896.
- 21. Anderson CB, Miller MJ, Murray AM, Fields TT, So NF, Christiansen CL. Falls After Dysvascular Transtibial Amputation: A Secondary Analysis of Falling Characteristics and Reduced Physical Performance. PM R. 2021;13(1):19-29. doi:10.1002/pmrj.12376.97 IJPN/Volume 13 Number 3, September-December 2025
- 22. Hunter SW, Batchelor F, Hill KD, Hill AM, Mackintosh S, Payne M. Risk Factors for Falls in People With a Lower Limb Amputation: A Systematic Review. PM R. 2017;9(2):170-180.e1. doi:10.1016/j.pmrj.2016.07.531.
- 23. Subedi B, Grossberg GT. Phantom limb pain: mechanisms and treatment approaches. Pain Res Treat. 2011;2011:864605. doi:10.1155/2011/864605.
- 24. Kumar A, Soliman N, Gan Z, et al. A systematic review of the prevalence of postamputation and chronic neuropathic pain associated with combat injury in military personnel. Pain. 2024;165(4):727-740. doi:10.1097/j. pain.0000000000003094.
- 25. van Schaik L, Geertzen JHB, Dijkstra PU, Dekker R. Metabolic costs of activities of daily living in persons with a lower limb amputation: A systematic review and meta- analysis. PLoS One. 2019;14(3):e0213256. Published 2019 Mar 20. doi:10.1371/journal.pone.0213256.
- 26. Göktepe AS, Cakir B, Yilmaz B, Yazicioglu K. Energy expenditure of walking with prostheses: comparison of three amputation levels. Prosthet Orthot Int. 2010;34(1):31-36. doi:10.3109/03093640903433928.
- 27. Toosizadeh N, Ehsani H, Miramonte M, Mohler J. Proprioceptive impairments in high fall risk older adults: the effect of mechanical calf vibration on postural balance. Biomed Eng Online. 2018;17(1):51. Published 2018 May 2. doi:10.1186/s12938-018-0482-8.
- 28. Kalff, M. N., Hoursch, V., Jopp, L., et al., (2024). Impact of Gait-Synchronized Vibrotactile Sensory Feedback on Gait in Lower Limb Amputees. Applied Sciences, 14(23), 11247. https://doi.org/10.3390/app142311247.
- 29. Petersen, Bailey (2023) Restoring Sensation After Lower-limb Amputations to Improve Balance and Gait. Doctoral Dissertation, University of Pittsburgh; 2023. Available at: https://dscholarship.pitt.edu/cgi/export/43759/ Text/d-scholarship-43759.txt. Last Accessed: 25/11/2025.
- 30. Karimi M, Yeganeh N, Makarov I, et al. Haptic Feedback Systems for Lower-Limb Prosthetic Applications: A Review of System Design, User Experience, and Clinical Insights. Bioengineering (Basel). 2025;12(9):989. Published 2025 Sep 18. doi:10.3390/ bioengineering12090989.
- 31. Zhu Y, Xia D, Zhang H. Using Wearable Sensors to Estimate Vertical Ground Reaction Force Based on a Transformer. Applied Sciences. 2023; 13(4):2136. https://doi.org/10.3390/ app13042136.
- 32. Wells ED, Shehata AW, Dawson MR, Carey JP, Hebert JS. Preliminary Evaluation of the Effect of Mechanotactile Feedback Location on Myoelectric Prosthesis Performance Using a Sensorized Prosthetic Hand. Sensors (Basel). 2022;22(10):3892. Published 2022 May 21. doi:10.3390/s22103892.
- 33. Chappell AG, Ramsey MD, Park S, Dumanian GA, Ko JH. Targeted Muscle Reinnervation-an Up-to-Date Review: Evidence, Indications, and Technique. Arch Plast Surg. 2025;52(3):153-168. Published 2025 Apr 1. doi:10.1055/a-2521-2199.
- 34. Baranwal N, Menville JE, Persad-Paisley EM, Sobti N, Kalliainen LK. Regenerative Peripheral Nerve Interfaces for the Management of Symptomatic Non-extremity Neuropathic Pain and Neuromas. Eplasty. 2024;24:e59. Published 2024 Oct 23.
- 35. Xu D, Wang Q. On-board Training Strategy for IMU-Based Real-Time Locomotion Recognition of Transtibial Amputees With Robotic Prostheses. Front Neurorobot. 2020;14:47. Published 2020 Oct 22. doi:10.3389/ fnbot.2020.00047.
- 36. Prasanna C, Realmuto J, Anderson A, Rombokas E, Klute G. Using Deep Learning Models to Predict Prosthetic Ankle Torque. Sensors (Basel). 2023;23(18):7712. Published 2023 Sep 6. doi:10.3390/s23187712. 37. Yang H, Liao Z, Zou H, et al. Machine learning-based gait adaptation dysfunction identification using CMill-based gait data. Front Neurorobot. 2024;18:1421401. Published 2024 Jul 29. doi:10.3389/fnbot.2024.1421401.
- 38. Wang Y, Wang Y, Mushtaq RT, Wei Q. Advancements in Soft Robotics: A Comprehensive Review on Actuation Methods, Materials, and Applications. Polymers. 2024; 16(8):1087. https://doi.org/10.3390/ polym16081087.
- 39. Perera O, Liyanapathirana R, Gargiulo G, Gunawardana U. A Review of Soft Robotic Actuators and Their Applications in Bioengineering, with an Emphasis on HASEL Actuators’ Future Potential. Actuators. 2024; 13(12):524. https:// doi.org/10.3390/act13120524.
- 40. Vassantachart AY, Yeo E, Chau B. Virtual and Augmented Reality-based Treatments for Phantom Limb Pain: A Systematic Review. Innov Clin Neurosci. 2022;19(10- 12):48-57. L. Lishma Shann Mathew, C. Vasantha Kalyani. From Artificial Limbs to Intelligent Limbs: Advances in Sensory-Enabled Prosthetic Technology98 International Journal of Practical Nursing IJPN/Volume 13 Number 3, September-December 2025
- 41. Viderman D, Tapinova G, Dossov T, Seitenov A, Abdildin T. Virtual reality for pain management: an umbrella review. Front Med (Lausanne). 2023;10: (2023). PMID: 37521355; PMCID: PMC10382225.
- 42. Arazpour M, Keshavarzi F, Gard SA. The effects of virtual reality environment simulations on balance and gait rehabilitation in persons with lower extremity amputation. Prosthet Orthot Int. Published online March 5, 2025. doi:10.1097/PXR.0000000000000428.
- 43. Hunt CL, Sun Y, Wang S, et al. Limb loading enhances skill transfer between augmented and physical reality tasks during limb loss rehabilitation. J Neuroeng Rehabil. 2023;20(1):16. Published 2023 Jan 27. doi:10.1186/s12984-023-01136-5.
- 44. Chang Y, Kang J, Cho H, Park S. A Comparative Study of the Effects of Augmented Reality Application on Movement Accuracy and Subjective Satisfaction in Rehabilitation Training for Individuals with Lower Limb Amputations. Applied Sciences. 2025; 15(12):6703. https://doi.org/10.3390/app15126703.
- 45. Sanz-Morère CB, Martini E, Meoni B, et al. Robot-mediated overground gait training for transfemoral amputees with a powered bilateral hip orthosis: a pilot study. J Neuroeng Rehabil. 2021;18(1):111. Published 2021 Jul 3. doi:10.1186/s12984-021-00902-7.
- 46. Koldaş Doğan Ş. Robot-assisted gait training in stroke. Turk J Phys Med Rehabil. 2024;70(3):293-299. Published 2024 Aug 26. doi:10.5606/tftrd.2024.15681
- 47. Villar Ortega E, Buetler KA, Aksöz EA, Marchal-Crespo L. Enhancing touch sensibility with sensory electrical stimulation and sensory retraining. J Neuroeng Rehabil. 2024;21(1):79. Published 2024 May 16. doi:10.1186/s12984- 024-01371-4.
- 48. AlQahtani NJ, Al-Naib I, Althobaiti M. Recent progress on smart lower prosthetic limbs: a comprehensive review on using EEG and fNIRS devices in rehabilitation. Front Bioeng Biotechnol. 2024;12:1454262. Published 2024 Aug 26. doi:10.3389/fbioe.2024.1454262.
- 49. Petrini FM, Bumbasirevic M, Valle G, et al. Sensory feedback restoration in leg amputees improves walking speed, metabolic cost and phantom pain. Nat Med. 2019;25(9):1356-1363. doi:10.1038/s41591-019-0567-3.
- 50. Thibaut A, Beaudart C, Maertens DE Noordhout B, Geers S, Kaux JF, Pelzer D. Impact of microprocessor prosthetic knee on mobility and quality of life in patients with lower limb amputation: a systematic review of the literature. Eur J Phys Rehabil Med. 2022;58(3):452-461. doi:10.23736/S1973- 9087.22.07238-0.
- 51. Chee L, Valle G, Marazzi M, et al. Optimallycalibrated non-invasive feedback improves amputees’ metabolic consumption, balance and walking confidence. J Neural Eng. 2022;19(4):10.1088/1741-2552/ac883b. Published 2022 Aug 25. doi:10.1088/1741- 2552/ac883b.
- 52. Graczyk EL, Resnik L, Schiefer MA, Schmitt MS, Tyler DJ. Home Use of a Neural- connected Sensory Prosthesis Provides the Functional and Psychosocial Experience of Having a Hand Again. Sci Rep. 2018;8(1):9866. Published 2018 Jun 29. doi:10.1038/s41598-018-26952-x.
- 53. Chen, C., Hanson, M., Chaturvedi, R. et al. Economic benefits of microprocessor controlled prosthetic knees: a modeling study. J NeuroEngineering Rehabil 15 (Suppl 1), 62 (2018). https://doi.org/10.1186/s12984-018- 0405-8.
- 54. Wijk U, Carlsson IK, Antfolk C, Björkman A, Rosén B. Sensory Feedback in Hand Prostheses: A Prospective Study of Everyday Use. Front Neurosci. 2020;14:663. Published 2020 Jul 7. doi:10.3389/fnins.2020.00663.
- 55. Donnelley CA, Shirley C, von Kaeppler EP, et al. Cost Analyses of Prosthetic Devices: A Systematic Review. Arch Phys Med Rehabil. 2021;102(7):1404-1415.e2. doi:10.1016/j. apmr.2021.02.010.
- 56. World Health Organization. WHO GATE (Global Cooperation on Assistive Technology) — access to assistive products is limited; only 1 in 10 in need has suitable access. WHO; 2017. Available at: https://www.who.int/ initiatives/global-cooperation-on-assistivetechnology-(gate). Last Accessed: 26/06/2025.
- 57. Htwe O, Yuliawiratman BS, Tannor AY, et al. Barriers and facilitators for increased accessibility to quality rehabilitation services in low- and middle-income countries: a systematic review. Eur J Phys Rehabil Med. 2024;60(3):514- 522. doi:10.23736/S1973- 9087.24.08154-1.
- 58. WHO Africa / Guidelines. Guidelines for training personnel and coverage of prosthetics & orthotics services — >75% of developing countries lack training programmes. WHO Regional Office materials; (training guidance). Available at: https://www.afro. who.int/sites/default/files/2017-06/who_guidelines_training_personnel_en.pdf?utm_ source=chatgpt.com. Last Accessed: 26/11/2025.
- 59. Clarke L, Puli L, Ridgewell E, Dillon MP, Anderson S. Regulation of the global orthotist/prosthetist workforce, and what we might learn from allied health professions with international-level regulatory support: a narrative review. Hum Resour Health. 2021;19(1):83. Published 2021 Jul 15. doi:10.1186/s12960-021-00625-9.
- 60. Jayaraman C, Mummidisetty CK, Albert MV, et al. Using a microprocessor knee (C- Leg) with appropriate foot transitioned individuals with dysvascular transfemoral amputations to higher performance levels: a longitudinal randomized clinical trial. J Neuroeng Rehabil. 2021;18(1):88. Published 2021 May 25. doi:10.1186/s12984-021-00879-3.
- 61. PrimeCare / industry summary and device reports on MPK maintenance, battery life and durability; technology reviews summarizing component lifetimes and maintenance burdens for bionic prostheses. (Industry/technical summary). 2024–2025. Available at: https:// www.robobionics.in/blog/how-long-dobionic-prosthetic-limbs-last-maintenanceand-durability-explained/. Last Accessed: 26/11/2025.
- 62. Gordon EC, Seth AK. Ethical considerations for the use of brain-computer interfaces for cognitive enhancement. PLoS Biol. 2024;22(10):e3002899. Published 2024 Oct 28. doi:10.1371/journal.pbio.3002899.
- 63. World Health Assembly / news coverage summarizing global commitments to scale rehabilitation and noting financing gaps that limit assistive technology scale-up. (News/WHO reporting). 2023. Available at: https://www.who.int/publications/i/ item/9789240049451. Last Accessed: 26/11/2025.
- 64. 3D printed prosthetics Global Market Report 2025. TBRC The Business Research Private Ltd. 2025. https:// www.thebusinessresearchcompany.com/ report/3d-printed- prosthetics-global-marketreport#:~:text=What%20Is%20The%203D%20 Printed,regulatory%20approvals%20a nd%20 quality%20standards.
- 65. Dallaev R. Advances in Materials with SelfHealing Properties: A Brief Review. Materials. 2024; 17(10): 2464. https://doi.org/10.3390/ ma17102464.
- 66. “Brain-controlled bionic limbs are inching closer to reality” — ScienceNews. Society for Science & the Public 2000–2025. 2024. Available at: https://www.sciencenews.org/article/ brain-controlled-bionic-limbs-anatomics. Last Accessed: 26/11/2025.
- 67. Jiang C, Xiao J, Wei H, Wang MY, Chen C. Review on Portable-Powered Lower Limb xoskeletons. Sensors (Basel). 2024;24(24):8090. Published 2024 Dec 18. doi:10.3390/s24248090.
- 68. Gardetto A, Müller-Putz GR, Eberlin KR, et al. Restoration of Genuine Sensation and Proprioception of Individual Fingers Following Transradial Amputation with Targeted Sensory Reinnervation as a Mechanoneural Interface. J Clin Med. 2025;14(2):417. Published 2025 Jan 10. doi:10.3390/jcm14020417.
- 69. Atallah H, Qufabz T, Naeem R, et al. The Current State of 3D-Printed Prostheses Clinical Outcomes: A Systematic Review. J Funct Biomater. 2025;16(10):370. Published 2025 Oct 1. doi:10.3390/jfb16100370. 70. Maiseli B, Abdalla AT, Massawe LV, et al. Braincomputer interface: trend, challenges, and threats. Brain Inform. 2023;10(1):20. Published 2023 Aug 4. doi:10.1186/s40708- 023-00199-3.
Data Sharing Statement
Funding
Author Contributions
Ethics Declaration
Acknowledgements
Conflicts of Interest
About this article
Cite this article
L. Lishma Shann Mathew, C. Vasantha Kalyani. From Artificial Limbs to Intelligent Limbs: Advances in SensoryEnabled Prosthetic Technology. Int J Practical Nurs. 2025; 13(3): 87-99.
Licence:
Attribution-Non-commercial 4.0 International (CC BY-NC 4.0)This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.
| Received | Accepted | Published |
|---|---|---|
| December 03, 2025 | January 08, 2025 | December 30, 2025 |
DOI: 10.21088 ijpn.2347.7083.13325.
Keywords
Prosthetic TechnologyNeural InterfacesMyoelectric ControlSensory FeedbackBiohybrid ProsthesesSearch for Similar Articles
Similar Articles
- Pilot Study to Evaluate the Effectiveness of Novel Designed Nebulizer (NDN) on P...
- Periodic Review of Benchmarks Contributing to Reduction of Healthcare Associate...
- A quasi Experimental Study to assess the effectiveness of Progressive Muscle Rel...
- KPI: A Performance Improvement Tool
- To assess the Effectiveness of Planned Teaching on Knowledge Regarding Preventio...
Article Level Metrics
Last UpdatedSaturday 28 February 2026, 18:18:37 (IST)
Accesses
Citations
Download citation
Article Keywords
Keyword Highlighting
Highlight selected keywords in the article text.
Timeline
| Received | December 03, 2025 |
| Accepted | January 08, 2025 |
| Published | December 30, 2025 |
licence
This license enables reusers to distribute, remix, adapt, and build upon the material in any medium or format for noncommercial purposes only, and only so long as attribution is given to the creator.